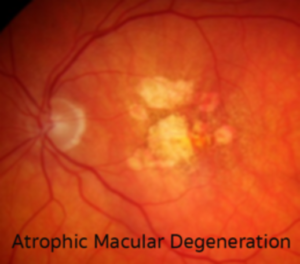
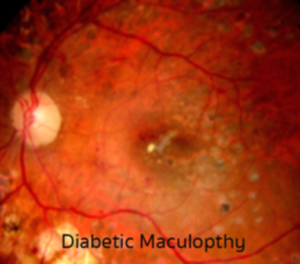
It has been observed clinically that, when anemia complicates systemic diseases such as leukemia or diabetes, there is often an exacerbation of attendant retinopathy with progressive appearance of ischemic lesions (nerve fiber layer infarcts, flame shaped hemorrhages) and more diffuse retinal microvascular leakage (edema secondary to diffuse telangiectasia with attendant capillary non-perfusion). Furthermore, when the anemia is treated with systemic administration of erythropoietin, it was observed that the lesions regressed, often with an improvement in vision. While this was thought initially to be due to the correction of the anemia, subsequent studies have demonstrated the erythropoietin glycoprotein to be a neural transmitter with receptors on retinal vascular endothelium, Mueller cells and RPE.
Intravitreal administration in diabetic animals results in a reduction of retinal vascular leakage predominantly of serum lipoproteins (through both a HIF 1 alpha inhibition of VEGF production and an anti-inflammatory inhibition of interlukins 1 and 6). The Mueller cells are activated, resulting in improved removal of the leaked lipoproteins and with the production of tissue neuroprotectants among which CNTF and BDNF have thus far been isolated. The result in the diabetic animal retina is an enhanced neuron survival in ischemia and edema models with reversal of neuron apoptosis and some regeneration. No ocular toxicity, angiogenesis, or systemic leakage has been observed in all animal or human studies.