A retrospective review was conducted of a cohort of sequential eyes with geographic atrophy threatening the fovea or with the fovea recently involved that were treated under a compassionate use off-label trial with compounded Procrit administered intravitreal, 5 IU every 6 weeks with complete ocular examinations performed at 6 week intervals and SDOCT, fluorescein angiography, and autofluorescence imaging, omnifield resolution perimetry every 3 months. SDOCT images were overlaid on the fluorescein angiograms and autofluorescence images and analyzed for loss of photoreceptor ellipsoid junction, loss of outer plexiform layer (OPL), and retinal pigment epithelium (RPE) redundancy or thickening. The primary outcome measure was rate of GA area progression during treatment compared with rates prior to treatment. Secondary outcomes were rate of GA progression in treated eyes compared GA progression when observed in the fellow eyes (without choroidal neovascularization), as well as the change in Omnifield Global Macular Acuity (GMA) during treatment compared with prior to treatment and compared with the fellow eye.
Results: 32 eyes of 28 patients were included, all of which had been followed for at least six months prior and then at least one year during treatment. The treated eyes often were the second to be involved with the GA and therefore started with slightly smaller GA (averaging 7.63+/- 7.56 mm2) compared with the fellow eye (8.59+/- 8.28 mm2) but enlarged prior to treatment at a faster rate (130+/-164%) than in the fellow eye (86+/-151%). During treatment the starting areas in the treated eyes were similar with those in the fellow eyes, but rate of area enlargement was reduced by 72% compared with a slowing of only 33% in the fellow eyes during the same period (which is the expected slowing of GA areas as they enlarge and coalesce with reduction in perimeter/area ratio. On Omnifield perimetry, the Global Macular Acuity during treatment improved an average of 0.12 logMAR (+/- 0.21) while in the fellow eyes an average loss of 0.14 logMAR(+/-0.27) was recorded. Among the treated eyes, 23% improved 0.3 logMar or greater compared with none of the fellow eyes. None of the treated eyes worsened 0.3 logMAR compared with 22% of the fellow eyes declining this degree
On SDOCT, disruption of the PEJ typically extended beyond the margins of geographic atrophy on overlaid fluorescein or autofluorescence images while RPE thickening often lined the margin. The best indicators of future GA progression were loss of OPL or loss of the PEJ. Omnifield perimetry scotomas corresponded with OCT loss of the OPL and PEJ.
Conclusions: Retrospective review of a small pilot study of compassionate use intravitreal Procrit appears to slow GA progression and central vision loss. SDOCT and Omnifield perimetry appear to be useful for mapping preserved retina and vision, monitoring disease progression, and predicting GA expansion.
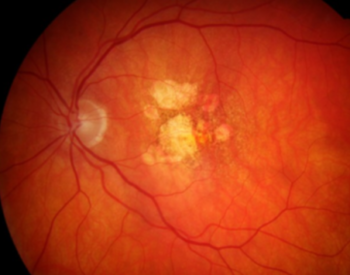
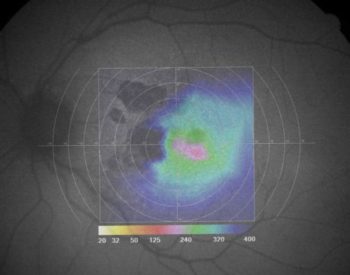
High contrast Omnifield resolution field of vision of the eye pictured above with juxtafoveal areas of geographic atrophy. Visual field has been inverted to demonstrate correlations.