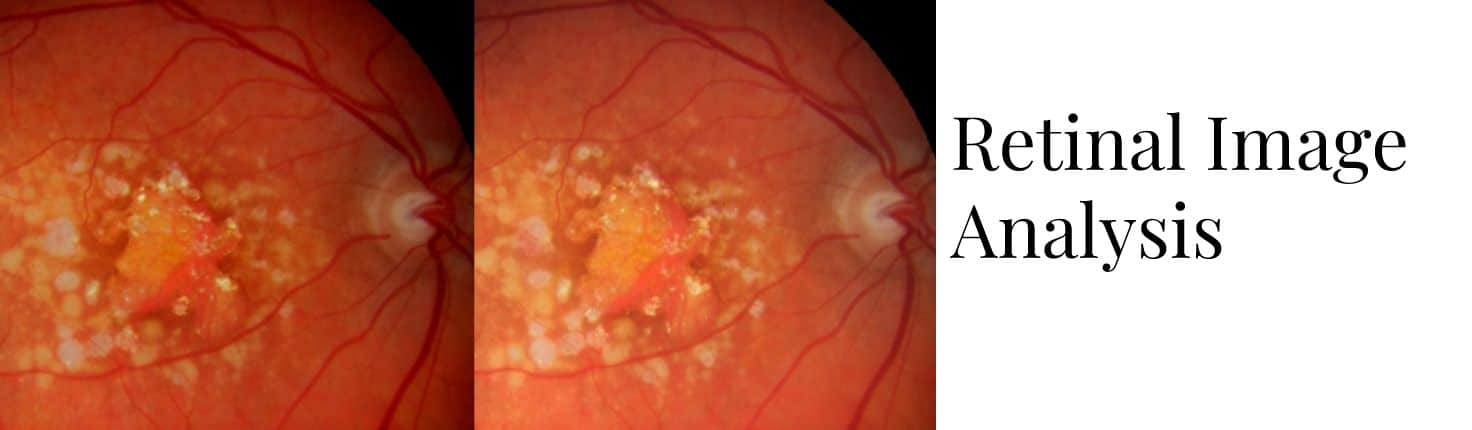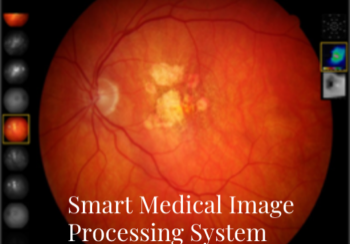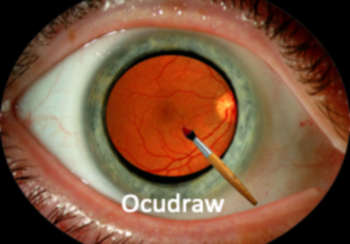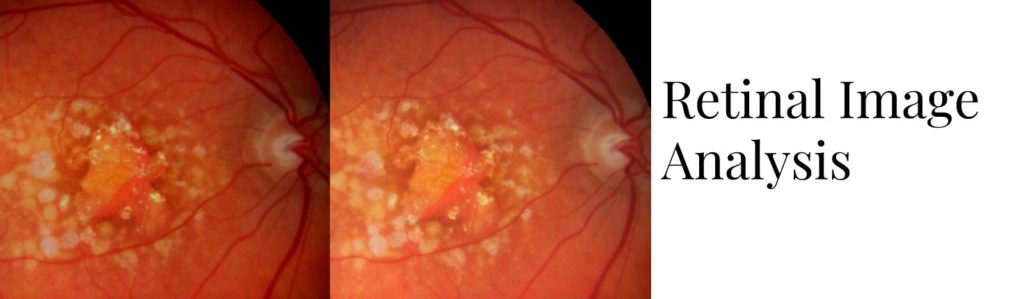
Macular diseases, have risen to become the major causes of moderate or severe vision impairment with severe disability, primarily because the detection of macular disease in the populations at risk is left to the traditional method of medical care delivery, in which the patient’s complaint of “blurred vision” initiates the care, and the retinopathy is most often discovered late in the course and only after there is significant, permanent, retinal injury, significant vision loss, and for whom in the vast majority of sufferers, vision cannot be adequately restored. Earlier detection of retinopathy requires a different paradigm of regular screening of the asymptomatic person, with recognition that retinal imaging, now achieved with cameras that do not require pupil dilation (enhancing patient compliance) significantly improves the detection of lesions. Vendor neutral systems that export the images from all manner of devices have allowed images to be reviewed by reviewers at centers or AI assisted systems, but this has been limited to generalized gradings of photographed vascular or RPE lesions. Furthermore, in the physician office, the images acquired over time are reviewed either sequentially or side by side, restricting the ability to identify changes. Furthermore, the observations are crudely entered into grades of the pathologic process. While image analysis systems have recently been developed with generated measurements (e.g. central retinal thickness, subretinal fluid thickness), for the most part they are directed only toward staging of the microangiopathy or RPE pathology and cannot evaluate individual lesion progression over time or association with visual field abnormalities because of lack of image overlay and registration.